The most common cause of pus in ear is otitis media (infection of the middle ear). The middle ear is the space between external and internal ear that contains air and 3 ear bones called ear ossicles. Anything that leads to bacterial invasion of the middle ear causes pus in ear.
Conditions Leading To Pus in Ear
There are certain conditions which can be caused by discharge from ear:
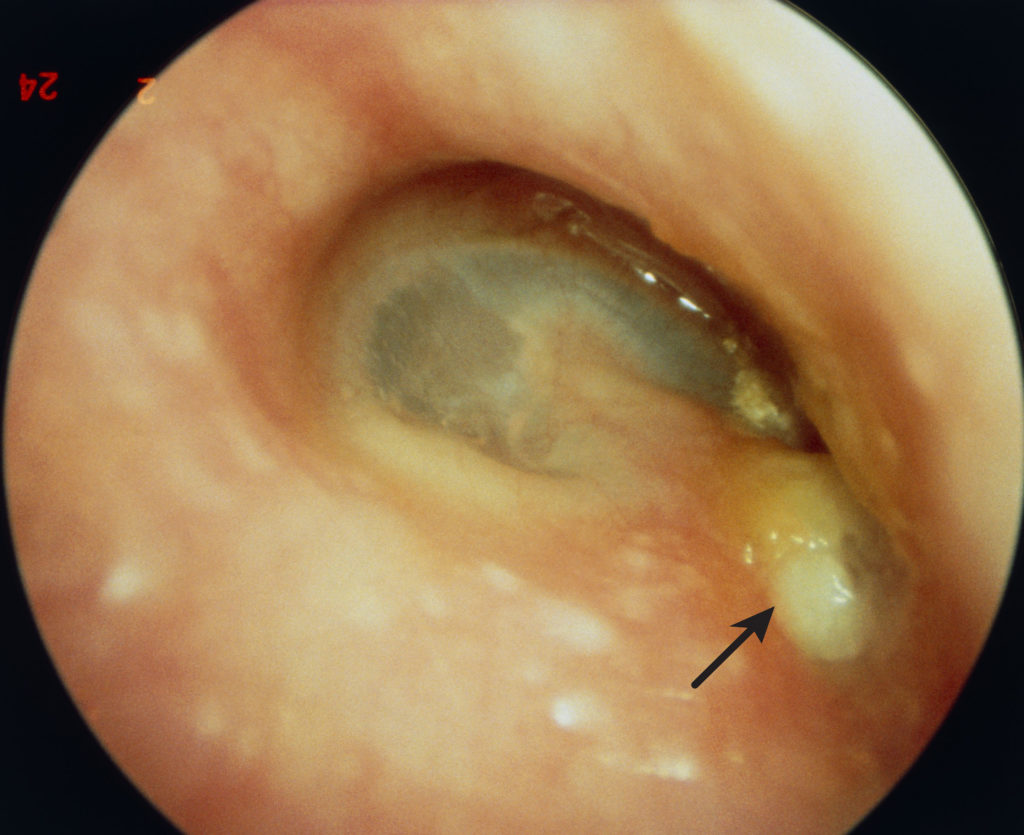
Acute suppurative otitis media:
It is an infection of the middle ear caused by pyogenic (pus-forming) bacteria. This is more common in children and lower socioeconomic groups. It usually occurs after upper respiratory tract infection e.g sore throat due to organisms invading the middle ear.
The main route of infection is the ‘Eustachian tube’ (tube containing middle ear and nose). It can also come from the external ear.
Acute necrotizing otitis media:
It is a type of otitis media in children and occurs after viral infections e.g. measles or influenza. It causes rapid destruction of the whole of the middle ear and eardrum.
Otitis media with effusion:
Also called ‘glue ear’ is an insidious condition characterized by an accumulation of pus in ear. The pus is thick and viscous but it can also be watery or thin. It affects children of 5-8 years of age. The eardrum is retracted and often appears dull or grey or blue in color and its mobility is restricted.
Chronic suppurative otitis media:
Named as CSOM is a long standing infection of the middle ear and is characterized by pus in ear and perforation of the eardrum. This usually occurs due to none healing of acute otitis media. It equally affects males and females and is the most common form of hearing loss in rural areas. It is of two types, Tubotympanic which has no serious complications and the other is Atticoantral which has a high risk of complications.
Tubercular otitis media:
It occurs secondary to pulmonary tuberculosis. The infection reaches the middle ear through the Eustachian tube and sometimes it is bloodborne. It is mostly seen in young adults and the process is slow. Multiple perforations occur in the middle ear and get filled with pus. The discharge from the ear is mostly painless.
What Are The Signs And Symptoms Of Pus In Ear?
A most common sign of middle ear infection is ear pain (otalgia). It may also present as
- Fever
- Rupture of eardrum
- Sinusitis (infection of nasal sinuses)
- Pain while lying down
- Sore throat
- Ringing or buzzing in the ear
- Hearing loss
- Bubbling of ear
What Causes Recurrent Pus in Ear?
Children: recurrent pus in ear occurs mostly in children of 6 months to 6 years old. Recurrent means 4-6 episodes of otitis media per year. The child remains symptom-free during the episodes. Feeding the baby without popping up the head may cause milk to enter the middle ear causing the ear infection and pus in ear.
Adults: in adults most common cause is recurrent sinusitis, pharyngeal insufficiency, infected tonsils, and immune deficiency.
How Long Pus In Ear Last?
In most cases, pus in ear lasts 3-5 days and resolves on its own without any specific treatment but in some cases, the infection lasts longer than 4 weeks and requires treatment. Some infections don’t even resolve after antibiotics for 6 weeks and surgery is required for such cases.
How Can Doctor Diagnose You?
Your doctor will ask your history and do your physical examination with special attention to your ears. He can examine you in the following ways
- Otoscope (an instrument to see eardrum)
- Audiometry, to see hearing loss
- Impedance audiometry, it is an objective test used in infants and children. The presence of fluid is indicated by this test.
- Tuning fork tests and vibration tests to check your hearing loss
- Culture and sensitivity of ear discharge
- X-ray mastoid process(bone behind the ear) will show cloudiness of air cells due to pus in ear
What Are The Predisposing Conditions Of Pus In Ear?
Anything that interferes with the normal functioning of the Eustachian tube predisposes to a middle ear infection. It can be due to
- Recurring attacks of common cold, viral infections like measles, influenza, diphtheria, and other respiratory tract infections.
- Infected tonsils
- Chronic rhinitis
- Nasal allergy
- Tumors of the nasal cavity or ear cavity
- Cleft palate
What Treatment Options Do You Have?
- Antibacterial therapy: it is indicated in all cases of pus with fever and severe ear pain. As the Discharge is due to bacterial invasion of the ear, it is important to treat them with antibiotics specific to the organism causing it. Antibacterial therapy is given for a minimum of 10 days till pus in ear resolves, eardrum heals and hearing returns to normal. Early discontinuance of antibiotics will lead to permanent hearing loss and earache.
- Decongestant nasal drops: these drops are applied inside the nose and they cause relief of nasal congestion and relieve swelling of the Eustachian tube and promote breathing.
- Oral decongestant drops: they achieve the same result as nasal drops but the only difference is that they are given orally.
- Analgesics and antipyretics: they help relieve fever and pain.
- Ear toilet: Discharge is mopped with sterile cotton bud and antibiotics are inserted.
- Local heat therapy helps to relieve pain.
- Myringotomy: it means incising eardrum to evacuate pus out of it and is indicated when the eardrum is swollen, bulging or bubbling and there is persistent pus in ear for more than 12 weeks.
- Mastoidectomy: it involves the removal of thick pus and surgical removal of mastoid pus.
What Are Sequelae Of Pus In Ear?
Persistent pus in ear can cause
- Eardrum rupture
- Ear bones destruction
- Fixation of ear bones
- Retraction pockets in ear
- Joint damage and fixation
- Hearing loss
- Tinnitus (buzzing in the ear)
- Vertigo (dizziness)
When to See Doctor?
If the pus in the ear lasts more than 3 days and is associated with fever, buzzing in ears, bulging of the eardrum, or sudden rupture of the eardrum, then you should not wait to seek medical help. Visit your nearby hospital to seek immediate medical help else delay in treatment can cause hazardous effects on-ear and cause permanent hearing loss.
HP Thoughts: Read about another incidence of ear pus here — Pus from Ear.







